Contact Us
Send as an email today!
-
Questions for Your Gastroenterologist
posted: Sep. 29, 2022.
Visiting a specialist, like a gastroenterologist, is a bit overwhelming if you're unsure of what to expect. However, when you visit the Digestive and Liver Center of Florida, serving Sanford, Read more -
Treatment Options for Hemorrhoids
posted: Jul. 27, 2022.
Want to get rid of your annoying hemorrhoids? Hemorrhoids are a common problem among men and women. The NIH reports that one in 20 Americans will deal with hemorrhoids, and as Read more -
Struggling With Acid Reflux?
posted: Jun. 08, 2022.

-
What Are the Warning Signs of Diverticulitis?
posted: May 25, 2022.

-
Who Should Get a Colonoscopy?
posted: Mar. 07, 2022.
-
Benefits Of Having A Gastroenterologist
posted: Jan. 11, 2022.
-
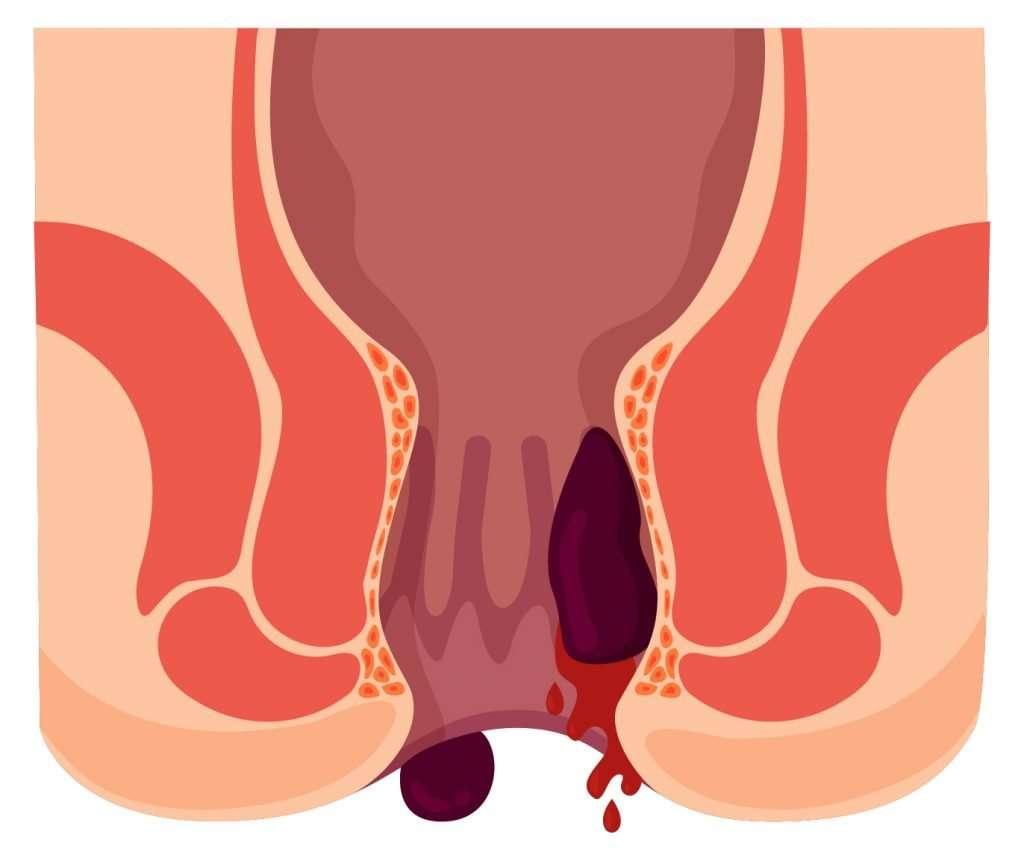
Signs And Symptoms Of Hemorrhoids
posted: Nov. 09, 2021.
-
Acid Reflux Symptoms and When to See a Gastroenterologist
posted: Oct. 14, 2021.
-
What Does a Gastroenterologist do?
posted: Oct. 14, 2021.
-
When To See Your Gastroenterologist For A Colonoscopy
posted: Sep. 22, 2021.
-
Choosing Your Gastroenterologist in Orlando
posted: Sep. 20, 2021.

-
Facts About Heartburn
posted: Aug. 18, 2021.

-
What Does it Mean to Have Lactose Intolerance?
posted: Jul. 28, 2021.

-
All You Need to Know About Foodborne Illness
posted: Jul. 20, 2021.
-
How Your Digestive System is Affected When You Smoke
posted: Jul. 12, 2021.

-
Whole Grains and Your Digestive System
posted: Jul. 07, 2021.

Contact Us
Our Locations
Find us on the map
Hours of Operation
For Kissimmee, West Orlando and Sanford Location: Please call our office for dates and times we will be at this location.
Orlando Office
Monday:
8:00 am-5:00 pm
Tuesday:
8:00 am-5:00 pm
Wednesday:
8:00 am-5:00 pm
Thursday:
8:00 am-5:00 pm
Friday:
8:00 am-5:00 pm
Saturday:
8:00 am-12:00 pm
Sunday:
Closed
Downtown Orlando
Monday:
8:00 am-5:00 pm
Tuesday:
8:00 am-5:00 pm
Wednesday:
8:00 am-5:00 pm
Thursday:
8:00 am-5:00 pm
Friday:
8:00 am-5:00 pm
Saturday:
Closed
Sunday:
Closed
